 
If the tracing persists with minimal or absent variability and there is no response to scalp stimulation or VAS for 60 minutes, the algorithm instructs the provider to deliver the infant because such a tracing is associated with significant acidemia. 26–28 Scalp stimulation or VAS should be performed every 20 minutes if there is no return of moderate variability. 25 However, scalp stimulation and VAS are easier to perform and have been shown to be reliable alternatives. Fetal scalp blood sampling (for pH) has long been used to assess fetal well-being. If the tracing is not associated with significant acidemia, then the algorithm instructs the provider to initiate conservative measures and to assess fetal well-being with scalp stimulation or VAS. 19,, 20,, 23,, 25 Such tracings should prompt the provider to proceed to delivery. The table on the bottom right side of Figure 2 lists relatively common FHR tracings associated with significant acidemia. If the tracing has recurrent variable decelerations (<90 beats per minute) or recurrent late decelerations with minimal or absent variability for 60 or more minutes, the management algorithm instructs the provider to deliver the infant because such a tracing is associated with significant acidemia. The yellow-coded section (dashed line and light grey box) addresses the management of a tracing with minimal or absent variability for 20 or more minutes. However, the notification guidelines instruct the registered nurse (RN) to notify the provider before 20 minutes have passed if the evolution of the tracing suggests that acidemia is developing quickly. 19,, 23,, 25 We believe that 20 minutes is a reasonable interval before notification because it allows at least 40 minutes before the tracing is significantly associated with acidemia. 19,, 20,, 23–25 The rapidity with which acidemia develops is influenced by the depth and length of the decelerations. 19,, 20 As a general rule, FHR variability gradually diminishes over a period of 60 to 120 minutes in association with recurrent late or variable deceleration as significant fetal acidemia develops. It includes tracings with decelerations or tachycardia because they are associated with fetal hypoxemia, 22 which can progress to acidemia, and it includes tracings with minimal or absent variability because they are significantly associated with acidemia if they persist for more than an hour. The yellow-coded section (dashed line and light grey box) addresses tracings that require provider notification within 20 minutes. There is no green-coded section (dotted line and box) as there is in the management algorithm because a complete listing of FHR tracings that do not require urgent provider (physician or certified nurse midwife ) notification would not be practical. The notification guidelines ( Figure 1) are laid out with the presenting tracing on the left and the recommended time before notification on the right. By allowing every member to make recommendations, SBAR flattens the labor and delivery (L&D) hierarchy, promoting the importance of multidisciplinary points of view and leading to greater patient safety.) Finally, they are both designed to fit on a single sheet of 8.5“x11” paper and are laminated and posted at multiple areas in L&D. It is succinct communication used between all members of the OB team when presenting patients. (Adapted from the military, SBAR stands for situation, background, assessment, and recommendation. 13,, 21 The wording in the tables differs slightly because the notification guidelines are geared to promote SBAR. 20 They both include tables that detail conservative measures, which are standard maneuvers that improve fetal status depending on the clinical situation. They emphasize the significance of moderate FHR variability because it is strongly associated with a pH >7.15 or newborn vigor, 19 and even with repetitive late or variable decelerations for one hour, its presence suggests a pH >7.10.  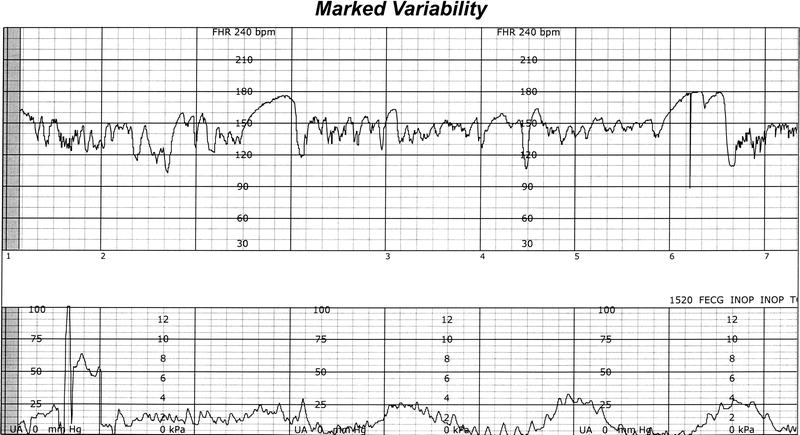
They are color coded in a manner similar to the familiar traffic light: green for FHR tracings that require attention but not urgently (indicated here by a dotted line box), yellow for tracings that require urgent attention (dashed line and a light grey box), and red for tracings that require emergent attention (solid line and dark grey box). It was our intent that they promote use of NICHD terminology and further communication within the obstetric (OB) team. The notification guidelines and management algorithm are designed to work in tandem in a multidisciplinary approach. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
